From Pilot to Scale: The Integration Playbook That Fuels Real Growth
Why innovation fails and how adaptive integration turns proof into performance.
Why Now: Pilots Are Not Enough
Healthcare doesn’t suffer from an innovation gap. It suffers from a scalability gap.
Across the industry, promising pilots rarely translate into enterprise value.
In 2024, nearly 40% of healthcare executives said that integration challenges directly hindered patient care and increased operating costs. Even more telling: 70% of digital health projects stall or fail because of workflow disruption, cost overruns, or poor adoption.
The pattern is consistent. Most pilots die within 6–12 months—not because the idea is weak, but because integration is brittle, costly, and slow.
This is not an innovation shortage. It’s an infrastructure failure.
The Reality Check: Hype Without Integration
AI has become the new gold rush. Large Language Models (LLMs) dominate headlines, and demos impress. But in healthcare, hype without infrastructure is fragile.
General-purpose AI models bring two structural risks:
Hallucination: They produce convincing but inaccurate or incomplete information. In clinical use, that risk is unacceptable.
Fragile Integration: Dropping an LLM into existing EMRs creates yet another bolt-on tool. It rarely aligns with workflow logic, payer rules, or compliance frameworks.
The result? Exciting pilots collapse at rollout.
Without architectural resilience, scale never happens.
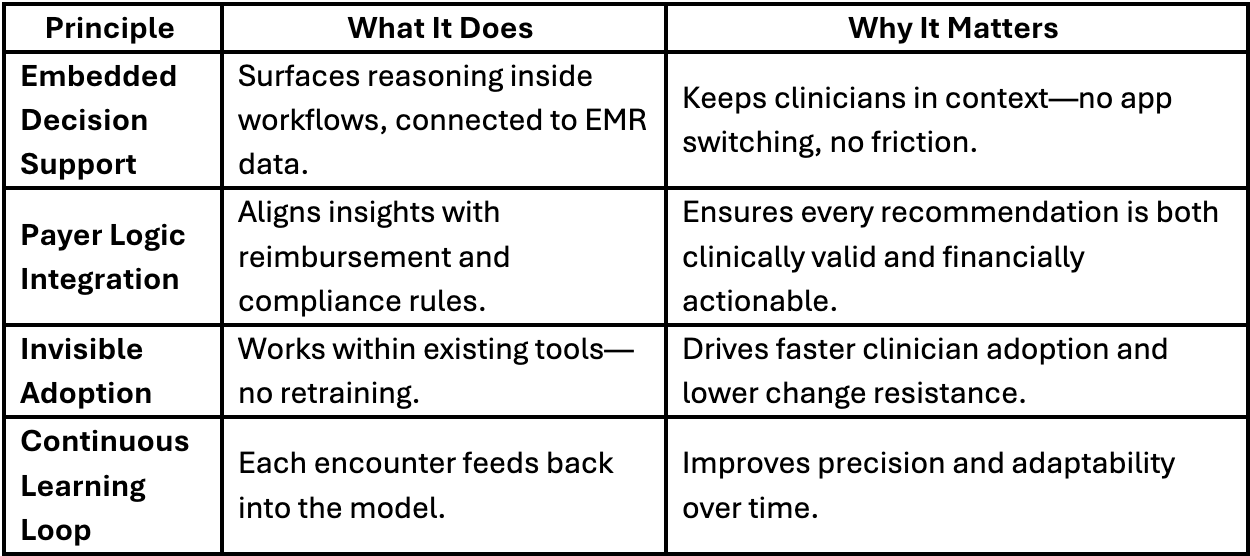
3. True Clinical Reasoning: Infrastructure for Intelligent Scale
At cliexa, we built True Clinical Reasoning to address exactly this. It’s a closed-loop intelligence system designed to make innovation scalable.
This is what turns proof-of-concept into durable growth. The AI hype cycle will fade, but infrastructure endures.
Systems that embed reasoning intelligence into their clinical, operational, and financial rails will scale sustainably long after the headlines move on.
The future of growth isn’t about buying bigger platforms. It’s about building systems that adapt as fast as your strategy changes.
Proof from the Field
Real-world evidence shows that integration design, not the technology itself, determines ROI:
Programs that embed tools directly into EHR workflows see up to 3× higher clinician adoption rates compared to standalone applications.
A leading U.S. health system cut integration costs by 40% by moving from one-off custom builds to a closed-loop model.
Another reduced time-to-scale from 18 months to 6 months, expanding AI-powered documentation system-wide with no additional training.
This is adaptive integration in action: less rework, faster rollout, stronger ROI.
Signals You Cannot Ignore
If these patterns sound familiar, your pilots may already be at risk:
IT teams buried under custom integration backlogs
High-value pilots stalling before full rollout
Clinician frustration from bolt-on tools that break workflows
Finance teams skeptical as costs climb while ROI stays unclear
Leadership Action Guide
CMIO / Clinical Innovation Leaders
Demand workflow-centric integration models that empower clinicians in design.
Evaluate adoption by workflow fit, not hours of training.
CIO / Interoperability Executives
Become architects of agility, not custodians of compliance.
Standardize around closed-loop frameworks to reduce tech debt and accelerate onboarding.
CFO / Finance Leaders
Track cost-per-rollout and stranded investments as balance sheet risks.
Adaptive integration shortens payback periods and minimizes stranded capital.
VP, Clinical Operations / Digital Strategy
Measure innovation by speed-to-value, how quickly pilots reach enterprise scale.
Remove IT bottlenecks so throughput gains aren’t lost in transition.
Looking 12–24 Months Ahead
The next two years will separate systems that innovate from those that integrate intelligently.
Early adopters will:
Cut pilot-to-scale timelines by 50% or more.
Protect budgets by avoiding stranded vendor costs.
Retain clinician trust through invisible, workflow-native design.
Gain first-mover advantage in the emerging modular care economy.
Laggards will:
Lose millions annually to failed integrations.
Watch clinician trust erode.
Miss the competitive window for scale and partnership-driven growth.
Call to Action
If interoperability is still treated as a compliance task in your organization, you’re leaving growth on the table.
Join the Real-Time Care Intelligence community to see how leading systems are:
Reducing integration debt
Scaling AI responsibly
Expanding partnerships without the rebuild cycle
👉 Take a 5 minute AI Assessment Quiz to see where your organization stands →
The future won’t wait for custom builds.
Let’s design systems that keep up.
Coming Next Week
Briefing 6: AI Doesn’t Need All the Data. It Needs the Right Data
I’ll explain why the future of AI in healthcare isn’t about amassing terabytes of information, but about curating the right data signals.